A platform that organizes and automates your provider enrollment process and keeps requirements visible and moving forward.











Our platform supports every stage of provider enrollment by keeping documentation visible, verification steps organized, and progress easy to monitor.
Monitor provider enrollment progress through intuitive dashboards that show submission status, pending steps, and verification updates.
Confirm credentials directly with official sources while maintaining organized records for easy future reference.
Track payer applications through structured workflows that help prevent delays and maintain clear submission timelines.
Store credential records securely in one location where authorized staff can quickly access them.
Generate enrollment reports that provide clear visibility into current credentialing progress.
Maintain updated provider information within centralized digital profiles that remain easy to review.
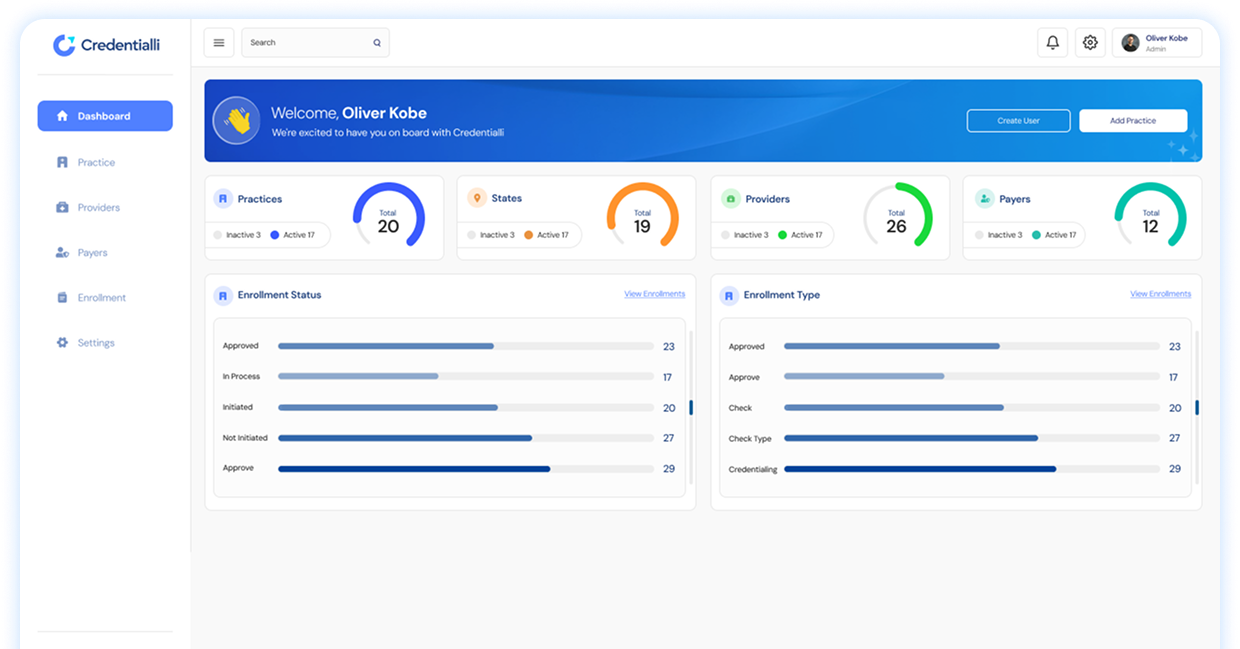
Are you exhausted because of the delays and confusion caused by unorganized credentialing? Our software aids medical practices in tracking provider applications, managing verification steps, and maintaining consistent visibility so administrators, credentialing teams, and leadership can take a breath of relief.
Our software also provides practical features that support streamlined administrative workflows.
Healthcare organizations trust our platform because it supports enrollment workflows with transparency, reliability, and consistent oversight.
Credentialing errors can occur when records are incomplete or scattered. Our solution helps maintain consistent documentation accuracy by organizing provider information in structured formats. This clarity reduces verification mistakes and supports reliable enrollment outcomes.
Credentialing usually requires collaboration across multiple administrative roles. Our software supports clear communication by keeping progress visible so teams remain aligned throughout enrollment workflows.

Healthcare organizations need predictable credentialing processes that remain consistent over time. Our system supports steady enrollment management so providers can transition into active roles without unnecessary uncertainty.

We don’t make false promises; we believe in showing tangible results.
Healthcare teams report saving an average of 10-14 administrative hours per week after implementing our software.
Organizations typically reduce credentialing timelines by 4 to 6 weeks per year with clearer visibility.
Our platform maintains a consistent 4.8/5 rating based on feedback from credentialing administrators.
Before using this software, we struggled to keep enrollment timelines clear. Now our team can instantly see provider status, which has reduced internal confusion and helped us maintain steady workflow progress.
Practice Administrator

The onboarding tools made a noticeable difference for our administrators. New providers complete requirements faster, and we spend far less time sending reminders or tracking missing paperwork.
Credentialli billing software has brought consistency and accuracy to our billing. We’ve seen a noticeable reduction in claim denials, and payments are processed more efficiently.
Credentialing Coordinator

Credentialing does not have to feel stressful or unpredictable. With the right system in place, your team can maintain stable progress, gain transparent oversight, and build stronger assurance at every stage of provider enrollment.
Let us simplify your credentialing workflow today!